STREAMD | Why Some Patients Are Paying $2,500 for a Better Recovery
Why Patients Are Paying Out of Pocket for a Concierge Surgical Experience
Something is shifting in how patients choose their surgeon.
For decades, the decision was largely logistical: which physician is in-network, which hospital is nearby, who has the next available appointment. Insurance coverage was the primary filter, and most patients assumed the care on the other side of that filter was roughly equivalent.
A growing number of patients are no longer making that assumption.
What concierge surgery actually looks like
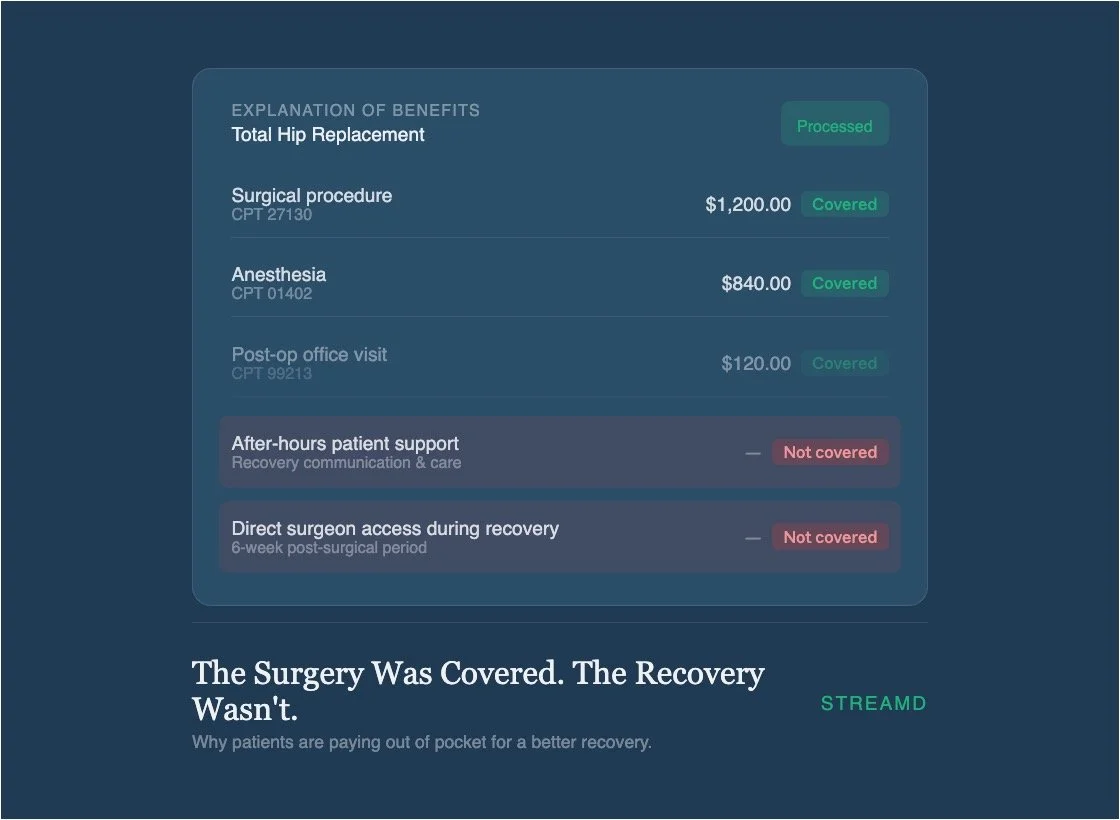
The concierge model in orthopedic surgery is not a new phenomenon, but it is expanding. Patients pay an out-of-pocket fee, typically ranging from $2,500 to $5,000, in exchange for a meaningfully different recovery experience. What that fee buys varies by practice, but the consistent elements are direct access to the surgeon, personalized communication throughout the recovery period, and a level of proactive support that the standard insurance-reimbursed model does not fund.
In practical terms, this means the surgeon calls the night before surgery. It means a patient who wakes at 3am worried about swelling gets an immediate, protocol-specific response rather than a voicemail. It means every post-operative appointment is with the surgeon who performed the procedure, not a rotating cast of mid-levels. It means someone is paying attention to the recovery, not just the operation.
For patients facing a major joint replacement, that distinction matters enormously.
Why insurance doesn't cover it
The reimbursement system pays surgeons for procedures, not for outcomes. A surgeon who invests heavily in patient communication, pre-operative education, and post-surgical support receives the same fee as one who does not. The system sends no signal that the investment is worth making, and over time, it produces predictable results: the infrastructure that improves outcomes gets cut because it cannot be sustained.
Concierge programs are, in part, a market correction to that structural failure. They allow surgeons who believe in a higher standard of perioperative care to build and maintain the infrastructure that supports it, funded by patients who understand the value of what they are paying for.
What the research says
This is not a luxury conversation without clinical stakes. Published research on enhanced surgical communication programs shows a 55% reduction in emergency department visits, a 40% reduction in hospital readmissions, and a 75% reduction in narcotic refill requests among patients enrolled in proactive, AI-powered recovery programs compared to standard care.
Patients in these programs also stop narcotics an average of 10 days sooner and report higher satisfaction scores across the board.
The concierge fee, in many cases, funds the program that keeps patients out of the emergency department. For a patient who avoids a single post-surgical complication, the out-of-pocket cost pays for itself many times over.
Who is choosing this and why
The patients choosing concierge surgical programs are not exclusively wealthy. They are, more precisely, patients who have done their research, who understand that surgical outcomes are not uniform, and who have decided that the recovery period is not where they want to cut costs.
Many have watched a family member struggle through a difficult recovery with insufficient support. Some are self-employed and cannot afford a prolonged or complicated recovery. Some simply value direct access to the physician who operated on them and are willing to pay for it.
What they share is an understanding that the surgical experience extends well beyond the operating room, and that the support structure around recovery is as important as the procedure itself.
What to look for
If you are considering a joint replacement and exploring whether a concierge program is right for you, the questions worth asking are straightforward. What does the surgeon's communication look like during recovery? Who handles post-operative concerns after hours? How many of your follow-up appointments will be with the surgeon personally? Is there a structured program to guide you through recovery milestones, or will you be largely on your own between visits?
The answers will tell you more about the quality of your recovery experience than any credential or ranking system.
Surgery is an hour. Recovery is months. It is worth knowing what happens after.
STREAMD is an AI-powered patient engagement platform built by orthopaedic surgeons for surgical practices. Learn more at ww.mystreamd.com